Kidney stones are hard deposits of minerals and salts that form inside the kidneys and can cause severe pain, urinary problems, and sometimes complications if left untreated.
What are kidney stones?
Kidney stones are solid, crystalline mineral deposits that form within the kidneys when certain substances in the urine, such as calcium, oxalate, uric acid, or cystine, become highly concentrated and crystallize. They vary in size, ranging from tiny grains that pass unnoticed in the urine to larger stones that can block the flow of urine and cause severe pain. Stones can form in one or both kidneys and may remain in the kidneys or travel down the urinary tract, sometimes lodging in the ureter, bladder, or urethra. The exact cause of kidney stone formation can vary, but risk factors include dehydration, dietary factors, obesity, certain medical conditions, and a family history of kidney stones. Symptoms often depend on the stone’s size and location. Small stones may cause no symptoms and pass unnoticed, while larger stones can result in sharp, cramping pain in the back or side, blood in the urine, nausea, vomiting, and frequent urination. Recurrent kidney stones can lead to more serious complications, including urinary tract infections or kidney damage if left untreated. Early detection, proper management, and preventive measures—such as adequate hydration and dietary modifications—play an essential role in minimizing discomfort and reducing the risk of future stones.
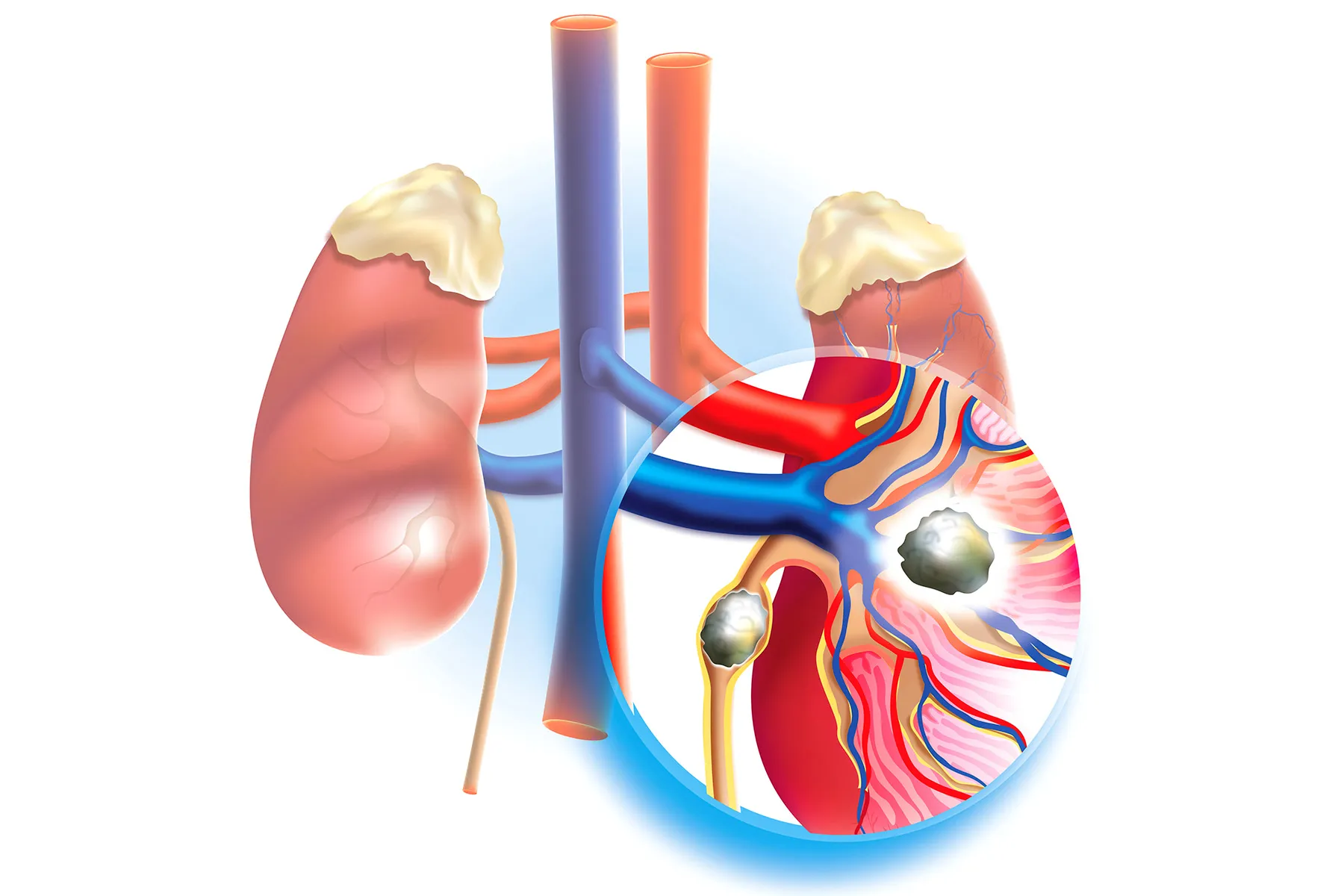
What are the types of kidney stones?
Kidney stones can be classified into several types based on their chemical composition, each with distinct causes and characteristics.
The most common type is calcium stones, which include calcium-oxalate and calcium phosphate stones. Calcium-oxalate stones form when calcium combines with oxalate in the urine, often influenced by diet, dehydration, or metabolic factors. Calcium phosphate stones are less common and may be associated with certain metabolic disorders or high urine pH.
Uric acid stones form when urine is consistently acidic, which can result from high-protein diets, gout, or dehydration. These stones are more likely to develop in people with low urine volume or those who excrete excess uric acid.
Struvite stones are typically linked to urinary tract infections caused by bacteria that produce urease, an enzyme that raises urine pH and promotes stone formation. These stones can grow rapidly and become quite large, sometimes forming staghorn-shaped stones that fill the kidney.
Cystine stones are rare and occur in people with a genetic disorder called cystinuria, which causes the kidneys to excrete excessive cystine, an amino acid that crystallizes in the urine.
Identifying the type of kidney stone is crucial for effective treatment and prevention, as each type may require different dietary modifications, medications, or interventions to reduce recurrence.

Who is at risk of developing kidney stones?
Certain individuals are at higher risk of developing kidney stones due to a combination of genetic, lifestyle, and medical factors.
Dehydration is one of the most significant risk factors, as low fluid intake reduces urine volume, allowing minerals to concentrate and crystallize. People who live in hot climates or engage in activities that cause excessive sweating may be particularly susceptible.
Dietary habits also influence risk: diets high in salt, sugar, animal protein, or foods rich in oxalate—such as spinach, nuts, and chocolate—can increase the likelihood of stone formation.
Medical conditions such as obesity, diabetes, gout, hyperparathyroidism, and inflammatory bowel disease can alter the body’s metabolism or urine composition, making stones more likely.
A family history of kidney stones significantly raises an individual’s risk, suggesting a genetic predisposition to stone formation.
Certain medications and supplements, including high-dose vitamin D, calcium supplements, and some diuretics, can also contribute.
Men are generally more prone to kidney stones than women, although the incidence in women has been increasing.
Age is another factor, with most kidney stones occurring in people between 30 and 60 years old.
Recognizing these risk factors can help individuals take preventive measures, such as staying hydrated, adjusting their diet, and managing underlying health conditions, to reduce the likelihood of stone formation.

How are kidney stones diagnosed?
Kidney stones are diagnosed through a combination of medical history, physical examination, and imaging or laboratory tests.
A healthcare provider will first review symptoms, which commonly include severe, cramping pain in the back or side, blood in the urine, frequent urination, nausea, or vomiting.
The doctor may also ask about risk factors, such as family history, diet, hydration habits, and previous kidney stones.
A urinalysis is often performed to detect blood, crystals, or signs of infection in the urine. Blood tests may also be used to check kidney function and identify elevated levels of calcium, uric acid, or other substances that contribute to stone formation.
Imaging plays a central role in confirming the presence, size, and location of kidney stones. Non-contrast CT scans are highly accurate and are considered the gold standard for detecting stones. Ultrasound is another common imaging method, particularly for patients who should avoid radiation, such as pregnant individuals. Less commonly, X-rays may be used, though some types of stones, like uric acid stones, are not easily visible on standard X-rays.
Identifying the stone’s size, type, and location is crucial for determining the appropriate treatment approach, whether it involves conservative management, medication, or surgical intervention, and for preventing future stones.
How are the kidney stones treated?
Kidney stone treatment depends on the stone’s size, type, location, and the severity of symptoms. Small stones often pass naturally through the urinary tract, and treatment focuses on relieving discomfort and facilitating passage.
This typically involves drinking plenty of water to help flush the stone, taking pain relievers to manage cramping, and sometimes using medications called alpha-blockers to relax the ureter and allow the stone to move more easily.
Larger stones, stones causing persistent pain, blockage, or infection, usually require medical intervention. Extracorporeal shock wave lithotripsy (ESWL) is a non-invasive procedure that uses sound waves to break stones into smaller fragments that can pass in the urine.
For stones lodged in the ureter or too large to pass, ureteroscopy may be performed, where a small scope is inserted into the urinary tract to remove or fragment the stone.
In more severe cases, percutaneous nephrolithotomy is used, involving a small incision in the back to remove large or complex stones directly from the kidney.
Following treatment, doctors may recommend dietary adjustments, medications, and lifestyle changes to prevent recurrence. Early intervention and appropriate treatment not only relieve pain but also reduce the risk of complications, such as urinary obstruction, infection, or kidney damage.

Conclusion
In conclusion, kidney stone treatment varies depending on the size, type, and location of the stone, as well as the severity of symptoms. Small stones may pass naturally with hydration, pain management, and medications to aid their movement, while larger or obstructive stones often require medical procedures such as shock wave lithotripsy, ureteroscopy, or percutaneous nephrolithotomy. Following treatment, preventive measures—including dietary adjustments, adequate hydration, and sometimes medication—are important to reduce the risk of recurrence.
Read More
