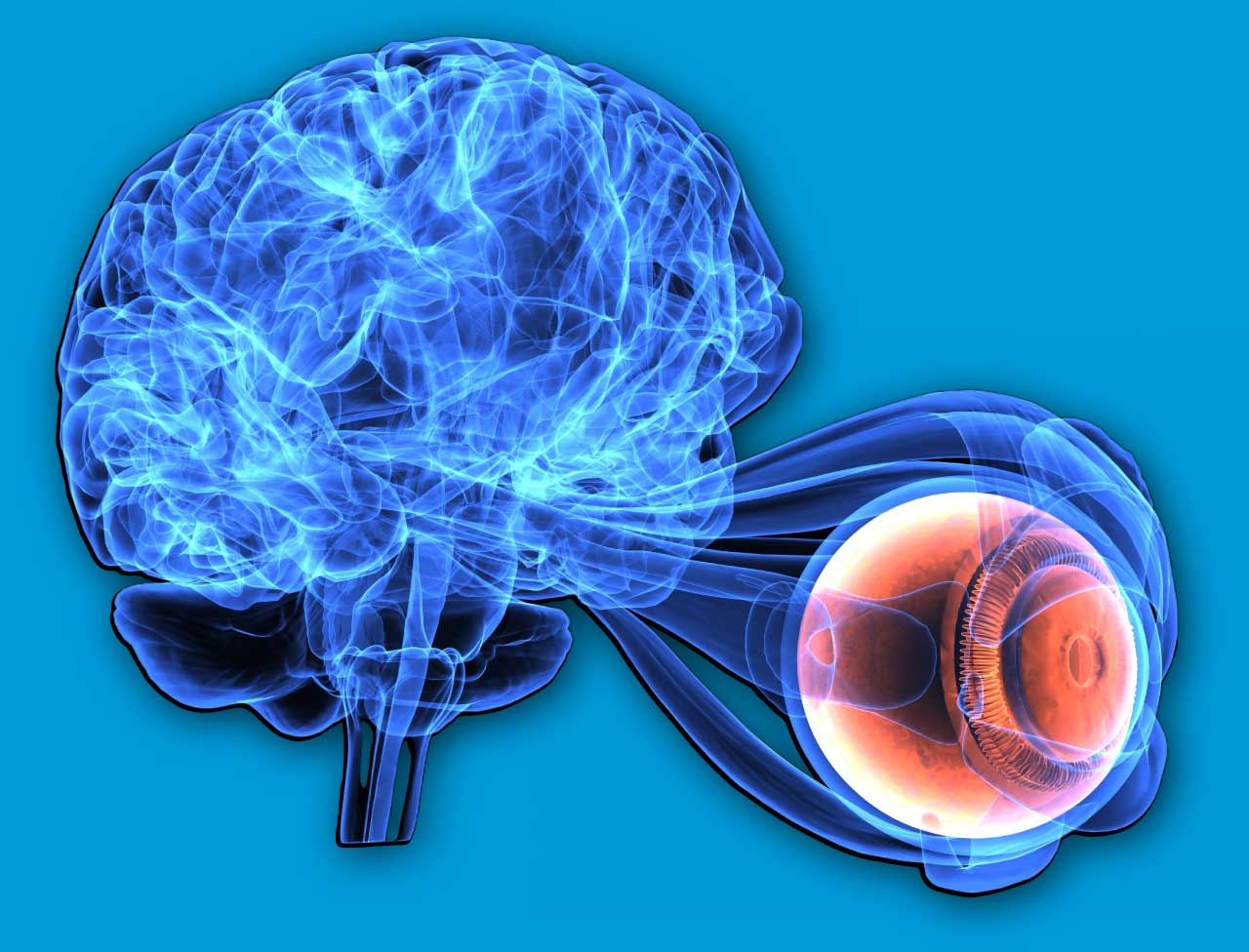
Neuro-ophthalmology is the intersection of neurology and ophthalmology that focuses on disorders of the visual system caused by disease of the optic nerve, visual pathways, ocular motor nerves, and the brain regions that control vision and eye movements.
What are the neuro-ophthalmic conditions?
Neuro‑ophthalmic conditions encompass a broad group of disorders in which visual symptoms arise from problems in the optic nerve, visual pathways, ocular motor nerves, neuromuscular junction, or brain regions that control eye movements and vision rather than from primary eye disease; these conditions therefore sit at the interface of neurology and ophthalmology and often require coordinated, multidisciplinary assessment.Clinically they present with a characteristic set of complaints and signs:
Abnormal movements of the eye (including nystagmus, saccadic intrusions, and ocular oscillations) reflect dysfunction of brainstem, cerebellar, or vestibular circuits and can be congenital, degenerative, toxic‑metabolic, inflammatory, or structural in origin;
Adult strabismus may be longstanding or acquired and when new in adulthood often signals cranial nerve palsy, myogenic disease, or central supranuclear causes and therefore warrants neuro‑ophthalmic evaluation;
Asymmetric pupils (anisocoria) or abnormal pupillary reactions point to afferent or efferent pathway lesions—from optic nerve disease producing a relative afferent pupillary defect to oculomotor or sympathetic pathway disruption producing ptosis and pupil asymmetry.
Double vision (diplopia) is a common and functionally disabling symptom that may result from isolated cranial nerve III, IV, or VI palsies, internuclear ophthalmoplegia, neuromuscular junction disorders, or central ocular motor pathway lesions; careful assessment of the pattern of diplopia (horizontal, vertical, torsional; worse in one gaze or with fatigue) helps localize the lesion.
Eyelid abnormalities such as ptosis, lid retraction, or lid lag can be caused by neuromuscular junction disorders.
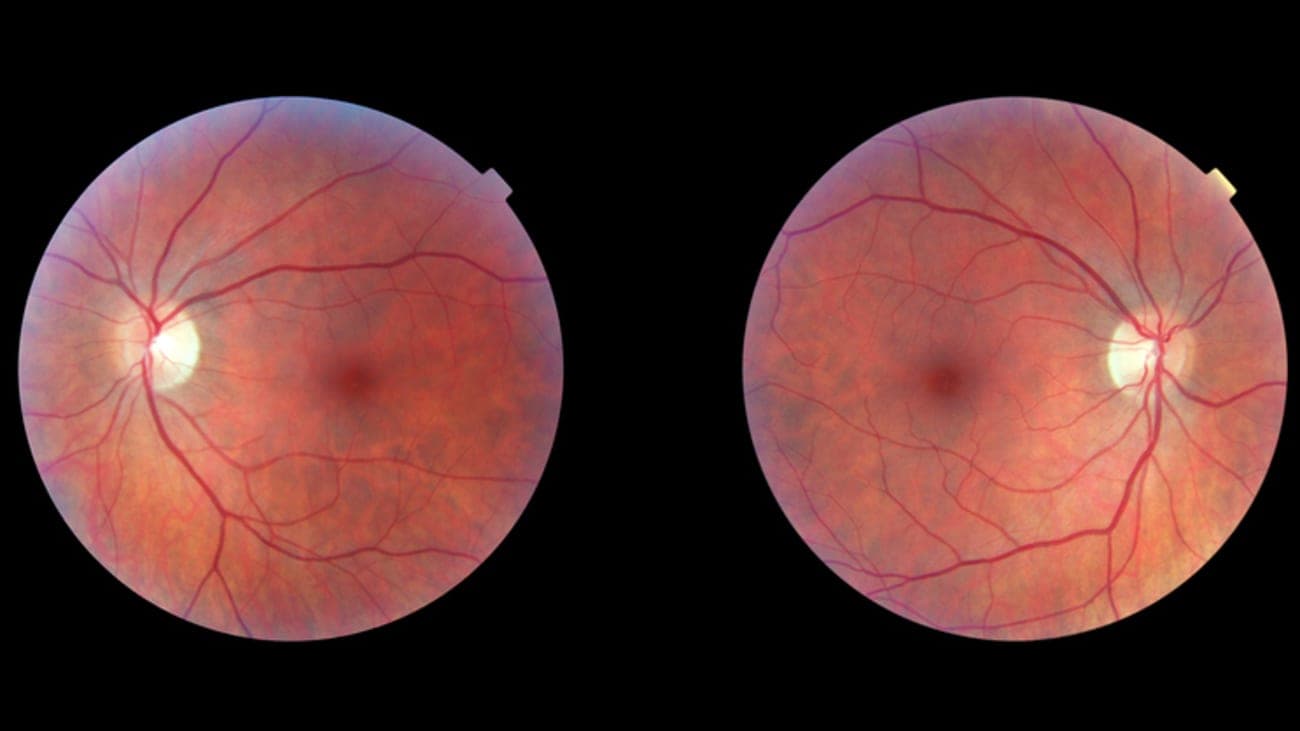
Optic nerve–related problems include optic neuritis, an inflammatory demyelinating optic neuropathy that typically causes subacute monocular vision loss, pain with eye movement, reduced color vision, and visual field defects and is closely associated with demyelinating diseases such as multiple sclerosis; prompt recognition is important because it guides investigations (MRI of the brain and orbits, serologic testing) and management decisions.
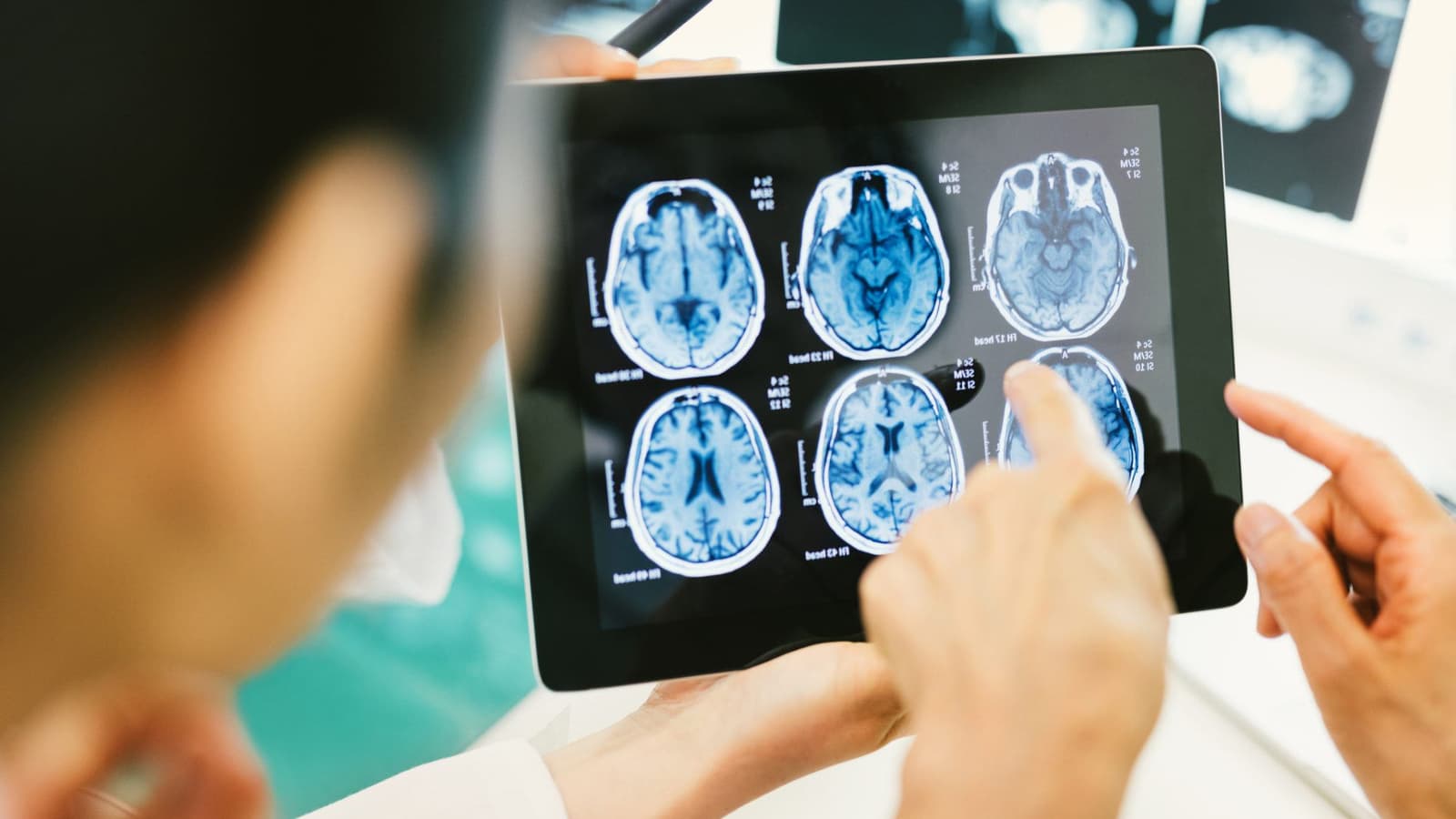
Across these conditions the diagnostic approach relies on a careful history and focused examination (visual acuity, color vision, pupils, ocular motility, cover testing, and funduscopy), targeted ancillary testing such as automated perimetry, optical coherence tomography, MRI of the brain and orbits with contrast, and laboratory or lumbar puncture studies when infection, inflammation, or raised intracranial pressure is suspected; timely recognition and referral are critical because many neuro‑ophthalmic disorders are treatable or require urgent intervention to preserve vision or address life‑threatening causes.
What causes neuro-ophthalmic conditions?
Neuro‑ophthalmic conditions arise from a wide range of causes that affect the optic nerve, visual pathways, ocular motor nerves, neuromuscular junction, or brain regions that control vision and eye movements; common categories include vascular events (ischemia, stroke, small‑vessel disease) that produce sudden vision loss or field defects, inflammatory and autoimmune disorders (optic neuritis, neuromyelitis optica, systemic vasculitis) that damage the optic nerve or visual pathways, and demyelinating diseases such as multiple sclerosis that frequently present with visual symptoms.Structural causes—compressive lesions from tumors, aneurysms, or orbital masses—can produce progressive optic neuropathy, proptosis, or cranial nerve palsies, while trauma and diffuse axonal injury cause direct optic nerve or cortical visual pathway damage.Infectious agents and postinfectious inflammation can inflame the optic nerve, and metabolic or toxic insults (nutritional deficiency, medications, toxins) produce optic neuropathies. Neuromuscular junction disorders like myasthenia gravis and endocrine‑related conditions such as thyroid eye disease cause fluctuating diplopia and eyelid signs, and raised intracranial pressure leads to papilledema and secondary visual loss. Genetic and congenital disorders, as well as degenerative neurologic diseases, complete the spectrum, so careful localization and targeted investigation are essential.
Conclusion
Neuro‑ophthalmic conditions bridge neurology and ophthalmology and demand careful localization, timely investigation, and coordinated care because they often signal treatable or urgent neurological disease. Early recognition of red flags—sudden vision loss, new diplopia with pupil involvement, rapidly progressive field loss, or signs of raised intracranial pressure—can preserve vision and identify life‑threatening causes. Management focuses on diagnosing the underlying etiology with targeted imaging and testing, treating reversible contributors, and involving multidisciplinary teams for long‑term rehabilitation and monitoring.
Read More