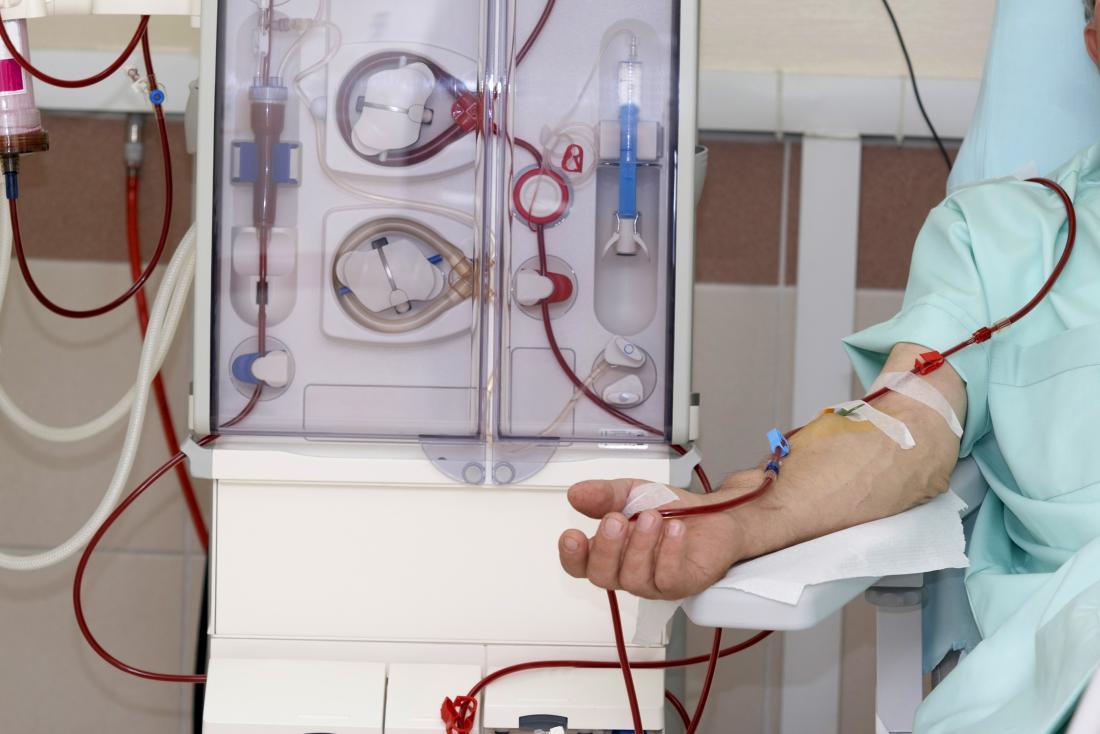
Dialysis is a life‑sustaining therapy that replaces the filtering functions of failed kidneys by removing waste, excess fluid, and correcting electrolyte imbalances.
What is Dialysis?
Dialysis is a medical treatment that replaces the filtering functions of failing kidneys by removing excess fluid, waste products, and balancing electrolytes and acid–base status when the native kidneys cannot do so adequately; it is used for acute kidney injury and for chronic kidney failure approaching or at end‑stage renal disease.There are two principal outpatient modalities—hemodialysis, which circulates blood through an external machine and dialyzer, and peritoneal dialysis, which uses the patient’s peritoneal membrane as a semi‑permeable filter by instilling and draining dialysate in the abdominal cavity—each with distinct technical requirements, lifestyle implications, and complication profiles.Dialysis can be delivered in-center or at home depending on the modality and patient factors, and in critically ill or hemodynamically unstable patients continuous renal replacement therapies provide gentler, continuous fluid and solute removal in intensive care settings.The decision to start and to choose a dialysis modality is individualized, based on symptoms, laboratory measures of kidney function, comorbidities, vascular access options, and patient preferences, and it aims to maintain life‑sustaining clearance while minimizing complications and preserving quality of life.
Who needs Dialysis?
Dialysis is indicated for people whose kidneys can no longer maintain fluid, electrolyte, and waste‑product balance sufficiently to sustain health; this includes patients with end‑stage kidney disease (chronic kidney failure) when conservative measures no longer control symptoms or metabolic derangements, and people with acute kidney injury who develop life‑threatening complications. Urgent indications include severe, refractory metabolic acidosis, dangerous electrolyte disturbances (notably hyperkalemia with ECG changes), volume overload causing pulmonary edema unresponsive to diuretics, symptomatic uremia (encephalopathy, pericarditis, intractable nausea), and certain toxic ingestions amenable to extracorporeal removal. Decisions to start chronic dialysis also consider symptoms (fatigue, anorexia, pruritus), declining clearance measures, nutritional status, comorbidities, and patient preferences; timing is individualized rather than based on a single lab threshold. In critically ill or hemodynamically unstable patients, continuous renal replacement therapies are chosen to provide gentler, continuous support. Some patients may opt for conservative, non‑dialytic management when dialysis would not meaningfully improve quality or duration of life.
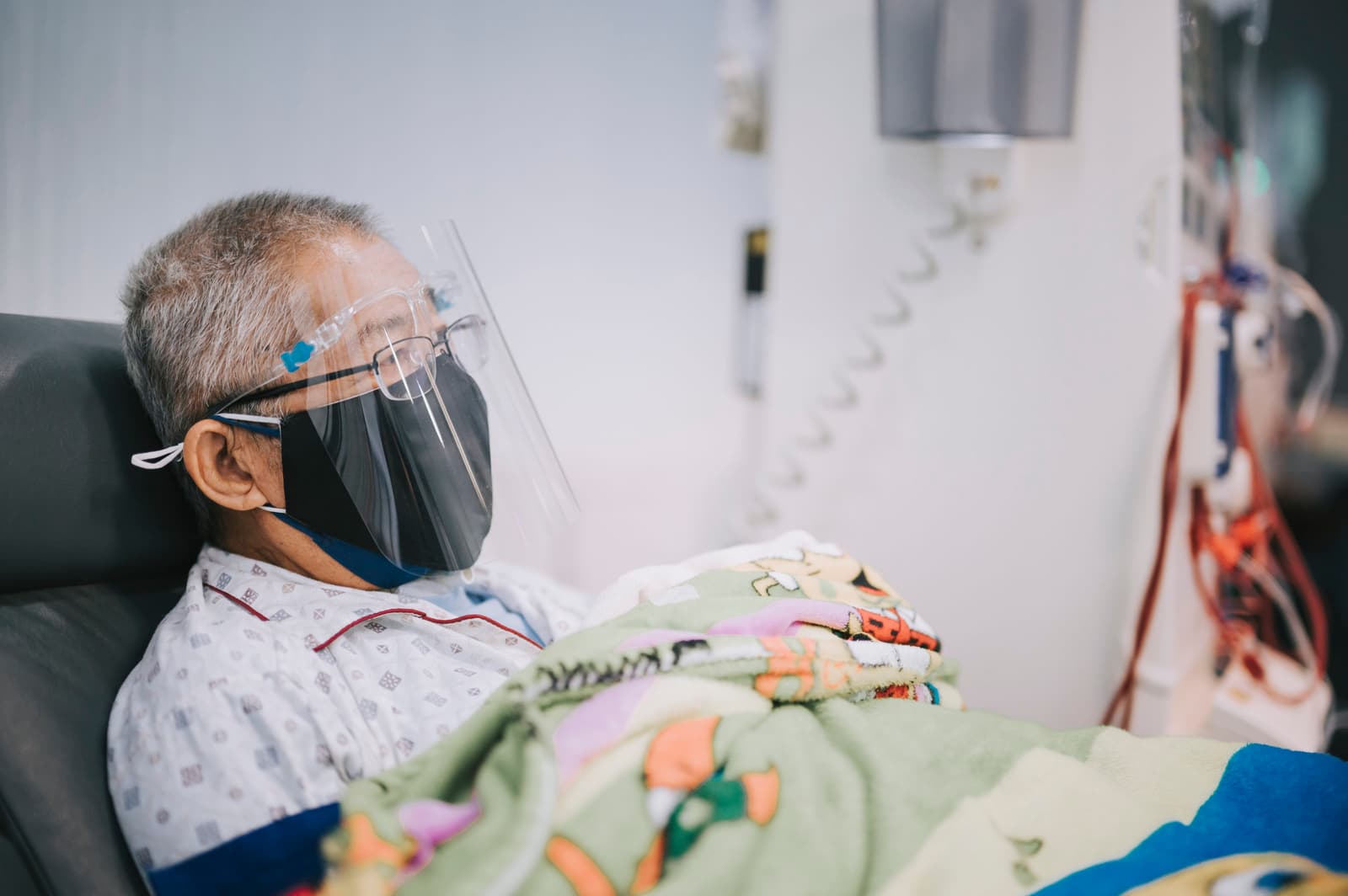
Types of Dialysis
Hemodialysis (HD), peritoneal dialysis (PD), continuous renal replacement therapy (CRRT), and hybrid approaches such as hemodiafiltration (HDF) or sustained low‑efficiency dialysis (SLED) represent the principal strategies for replacing kidney function, each with distinct mechanisms, settings, and clinical trade‑offs:
Hemodialysis uses an extracorporeal circuit to pump blood through a dialyzer where solute diffusion and ultrafiltration across a semipermeable membrane remove toxins and excess fluid, is commonly delivered intermittently in a center (typically three times weekly) or at home with specialized equipment, requires reliable vascular access (arteriovenous fistula, graft, or catheter), and is favored for its rapid clearance and standardized monitoring but can cause hemodynamic shifts and requires travel or home training.
Peritoneal dialysis leverages the patient’s peritoneal membrane as the dialysis surface by instilling dialysate into the abdominal cavity and allowing solute and fluid exchange over dwell times; it can be performed as continuous ambulatory PD (CAPD) or automated PD (APD) overnight, offers greater independence and more continuous metabolic control, and is often chosen for lifestyle reasons or preserved vascular access, though it carries risks of peritonitis, catheter complications, and limitations in ultrafiltration for some patients.
In critically ill or hemodynamically unstable patients, CRRT provides slow, continuous removal of solutes and fluid over 24 hours using convective, diffusive, or combined modalities (continuous venovenous hemofiltration, hemodialysis, or hemodiafiltration) and is delivered in the intensive care unit to minimize abrupt volume shifts and support gradual metabolic correction while allowing concurrent hemodynamic and organ support.
Hybrid and alternative strategies bridge the gap between intermittent and continuous therapies: hemodiafiltration (HDF) combines diffusive dialysis with convective clearance to enhance removal of middle‑molecular‑weight toxins and may be delivered online in high‑flux hemodialysis units, while SLED (sustained low‑efficiency dialysis) applies prolonged, lower‑flow hemodialysis sessions—often 6–12 hours—using conventional dialysis machines in the ICU to achieve gentler hemodynamic profiles without the resource intensity of CRRT; these hybrid approaches are selected based on patient stability, soluteremoval goals, and local resources.
Which type of dialysis do I need?
Choosing among modalities requires balancing clinical factors (hemodynamic status, residual kidney function, comorbidities, infection risk), practical considerations (availability of home support, training capacity, vascular access options), and patient preferences (work, travel, and quality‑of‑life priorities); for example, PD may preserve lifestyle flexibility and vascular access but demands patient engagement and infection vigilance, whereas in‑center HD centralizes care and monitoring but imposes a fixed schedule and potential intradialytic symptoms.Technical and safety considerations also shape modality choice: vascular access planning and infection prevention are critical for HD, catheter care and sterile technique are essential for PD, anticoagulation and filter management are routine in CRRT, and water quality, machine capabilities, and staffing influence the feasibility of HDF or SLED.Ultimately, optimal dialysis care is individualized and dynamic—patients may transition between modalities over time (for example, starting with CRRT in the ICU, moving to SLED or intermittent HD as stability improves, or electing PD for home‑based chronic therapy)—and shared decision‑making with nephrology, nursing, and allied teams ensures that the chosen modality aligns with clinical needs, safety imperatives, and the patient’s life goals.
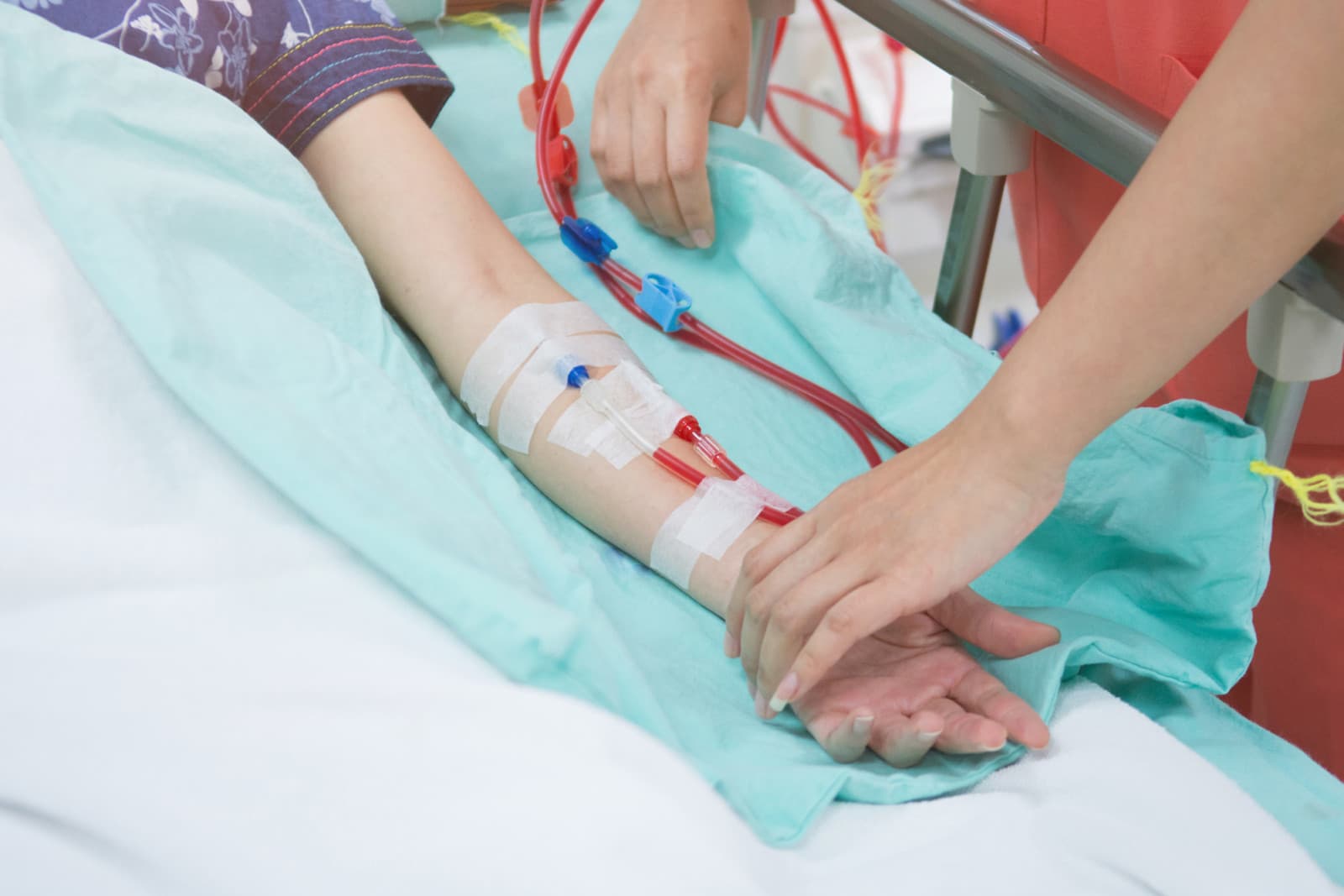
Conclusion
Dialysis offers multiple, effective ways to replace kidney function—hemodialysis, peritoneal dialysis, continuous renal replacement therapy, and hybrid approaches like hemodiafiltration or SLED—each tailored to different clinical needs, patient lifestyles, and care settings. Choosing the right modality balances medical factors (hemodynamic stability, residual kidney function, comorbidities), practical considerations (access, home support, resource availability), and personal preferences. Early planning, careful vascular or catheter management, infection prevention, and ongoing collaboration between patients and the nephrology team optimize safety and quality of life. Patients may transition between modalities over time as their condition and goals change, and shared decision‑making ensures the selected approach aligns with both clinical priorities and daily living needs.
Read More