Labiaplasty is a surgical procedure designed to reshape or reduce the size of the labia minora (the inner vaginal lips), and in some cases the labia majora (the outer vaginal lips).
What is Labiaplasty?
Labiaplasty is a surgical procedure that alters the size, shape, or symmetry of the labia, most commonly the labia minora, which are the inner folds of skin surrounding the vaginal opening. The procedure is performed for a variety of reasons, including physical comfort, functional concerns, and personal or aesthetic preferences. Some individuals experience irritation, discomfort, or pain during activities such as exercise, sexual intercourse, or wearing tight clothing due to enlarged or uneven labia. Others may seek labiaplasty to address changes resulting from childbirth, aging, hormonal influences, or natural anatomical variation. Labiaplasty is a highly individualized procedure, with surgical techniques tailored to each patient’s anatomy and goals, aiming to achieve a natural appearance while preserving sensation and function. It is typically performed on an outpatient basis under local or general anesthesia, with most patients able to return to normal daily activities within a few days, although full healing may take several weeks. As with any surgical procedure, labiaplasty carries potential risks and benefits, which should be carefully discussed during a thorough consultation with a qualified healthcare provider. When appropriately indicated and skillfully performed, labiaplasty can improve physical comfort, self-confidence, and overall quality of life.

Why would someone get a labiaplasty?
Someone may choose to undergo labiaplasty for a range of medical, physical, cosmetic, emotional, and reconstructive reasons, often overlapping rather than existing in isolation.
From a medical or physical standpoint, enlarged or asymmetrical labia can cause chronic irritation, pain, or chafing during activities such as exercise, cycling, sexual intercourse, or prolonged sitting, and may contribute to recurrent infections or hygiene difficulties. Addressing these issues can significantly improve daily comfort and physical well-being.
Cosmetic and emotional reasons are also common, as some individuals feel self-conscious or distressed about the appearance of their genital anatomy due to natural variation, aging, childbirth, or societal influences. This discomfort can affect self-esteem, intimate relationships, and overall confidence, and labiaplasty may help alleviate these concerns when expectations are realistic and patient-driven.
In addition, labiaplasty may be performed as reconstructive surgery following trauma, injury, congenital conditions, or previous surgical complications, with the goal of restoring both form and function.
In all cases, the decision to pursue labiaplasty is highly personal and should be made after careful consideration, thorough consultation, and a clear understanding of the potential benefits, risks, and limitations of the procedure.
What causes a labium to become oversized?
Oversized or elongated labia, particularly the labia minora, are most often the result of natural anatomical variation and are not inherently abnormal.
Genetics play a significant role, as labial size, shape, and symmetry vary widely among individuals from birth.
Hormonal changes can also influence labial tissue, especially during puberty, pregnancy, and menopause, when fluctuations in estrogen levels may cause the labia to grow, stretch, or change in elasticity.
Childbirth is another common factor, as vaginal delivery can place tension on the labial tissue, sometimes leading to elongation or asymmetry.
Aging contributes as well, since skin and connective tissue naturally lose firmness and elasticity over time.
In some cases, chronic friction or pressure from activities such as cycling, horseback riding, or wearing tight clothing may contribute to gradual stretching of the labia.
Less commonly, oversized labia may result from trauma, injury, inflammation, or certain medical or congenital conditions affecting tissue growth.
It is important to note that labial enlargement is usually benign and does not indicate a health problem on its own.
Concerns typically arise only when size or shape causes physical discomfort, hygiene difficulties, or emotional distress, at which point evaluation by a qualified healthcare provider may be helpful.

What is the average age for labiaplasty?
There is no single “average” age for labiaplasty, as the procedure is sought by individuals across a wide adult age range for different reasons and life circumstances. Most patients who undergo labiaplasty are adults between their early 20s and late 40s, although some seek the procedure earlier or later depending on their needs. Younger adults may pursue labiaplasty after puberty once genital development is complete, often due to lifelong discomfort, irritation during physical activity, or long-standing concerns about labial appearance. Others consider the procedure later in life following childbirth, hormonal changes, or aging, which can affect labial size, symmetry, and tissue elasticity. It is generally recommended that labiaplasty be performed only after full physical maturity to ensure stable anatomy and informed decision-making. In rare cases involving significant functional impairment or congenital conditions, surgery may be considered at a younger age, but this requires careful ethical consideration, medical necessity, and involvement of appropriate guardians and healthcare professionals.

What happens before surgery?
Before labiaplasty surgery, patients undergo a comprehensive consultation and preparation process to ensure the procedure is appropriate, safe, and aligned with their goals. This begins with a detailed medical history review, including current medications, allergies, previous surgeries, and any underlying health conditions. The surgeon will perform a physical examination to assess anatomy and discuss concerns, expectations, and desired outcomes, while also explaining the available surgical techniques and potential risks. Preoperative photographs may be taken for medical documentation with the patient’s consent. Patients are typically advised to stop smoking and avoid certain medications or supplements, such as aspirin or anti-inflammatory drugs, that can increase bleeding. Pre-surgical instructions may also include guidelines on hygiene, fasting if anesthesia is planned, and arranging transportation and post-operative support. In some cases, laboratory tests or medical clearance from a primary care provider may be required. Clear communication is emphasized so patients understand the recovery process, potential discomfort, and realistic results. This preparatory phase is essential for optimizing surgical outcomes, minimizing complications, and ensuring patients feel informed, confident, and emotionally prepared before undergoing labiaplasty.

What happens during labiaplasty?
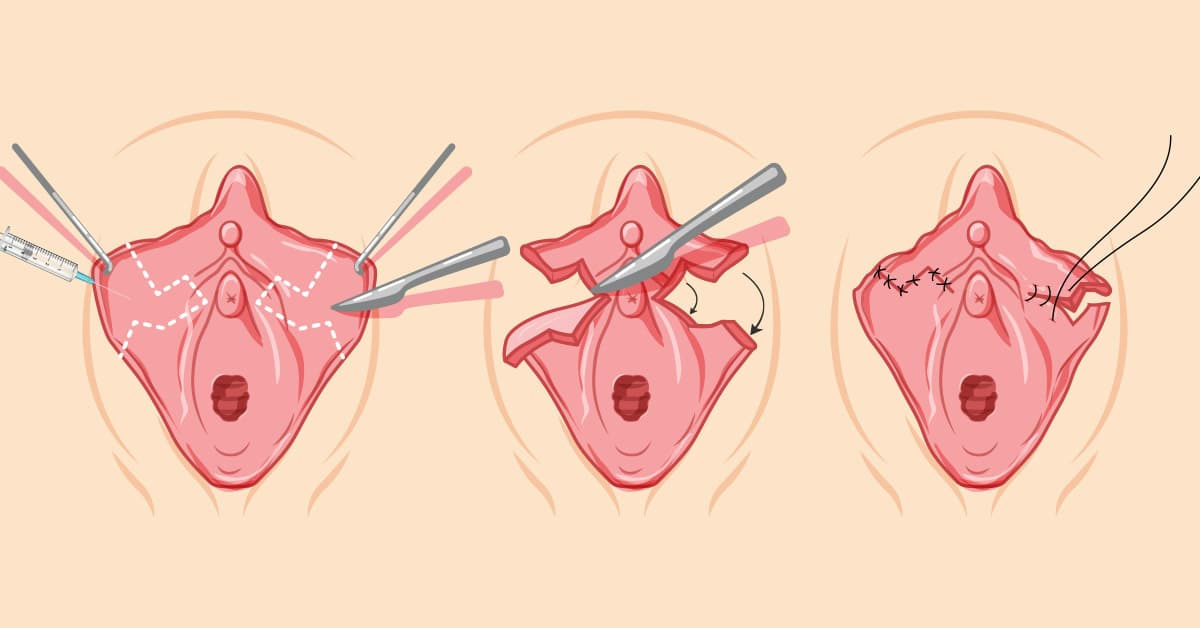
During labiaplasty, the procedure is performed in a controlled surgical setting with a focus on precision, safety, and preservation of normal function. It is typically done on an outpatient basis under local anesthesia with sedation or general anesthesia, depending on the patient’s needs and the extent of surgery. Once anesthesia takes effect, the surgeon carefully marks the treatment area to guide tissue removal or reshaping. Excess labial tissue is then reduced using a chosen surgical technique, such as the trim method or wedge method, each selected based on the patient’s anatomy and desired outcome. The goal is to create a natural appearance while maintaining symmetry, sensation, and blood supply. Meticulous surgical technique is essential, as the labial area is highly sensitive and vascular. After reshaping, the incisions are closed with fine, absorbable sutures that do not require removal. The entire procedure typically lasts one to two hours. Once completed, the patient is monitored briefly before being discharged the same day with detailed aftercare instructions. Mild swelling, bruising, and discomfort are common initially and are managed with medication and rest. Overall, labiaplasty is designed to improve comfort and aesthetics while prioritizing safety and long-term function.

Labiaplasty Recovery process
The labiaplasty recovery process varies slightly from person to person but generally follows a predictable course focused on healing, comfort, and gradual return to normal activities.
In the first few days after surgery, patients can expect swelling, bruising, and mild to moderate discomfort, which are typically managed with prescribed pain medication, cold compresses, and rest.
Keeping the surgical area clean and dry is essential, and patients are usually given specific hygiene instructions to reduce the risk of infection.
Most individuals are able to resume light daily activities within a few days, although strenuous exercise, sexual activity, and activities that place pressure on the area should be avoided for several weeks.
Swelling gradually decreases over the first two to four weeks, but subtle swelling may persist longer as the tissues continue to heal.
Dissolvable sutures are commonly used and will naturally fall out as healing progresses.
Follow-up appointments allow the surgeon to monitor recovery and address any concerns. Full healing and final results typically become apparent after several weeks to a few months.
Adhering closely to post-operative instructions is crucial for optimal healing, minimizing complications, and achieving the best possible functional and aesthetic outcome.

What are the risks and complications of labia surgery?
As with any surgical procedure, labiaplasty carries potential risks and complications, although serious issues are uncommon when the surgery is performed by a qualified and experienced surgeon.
Common short-term risks include swelling, bruising, bleeding, and temporary discomfort, which are generally part of the normal healing process.
Infection is a possible complication, but it is rare when proper surgical technique and post-operative care are followed.
Some patients may experience delayed wound healing or minor wound separation due to tension in the area or excessive activity during recovery.
Changes in sensation, such as temporary numbness or increased sensitivity, can occur and usually resolve over time, though permanent sensory changes are rare.
Scarring is typically minimal and well concealed, but in some cases, noticeable or uncomfortable scar tissue may develop.
Asymmetry or dissatisfaction with cosmetic results is another potential risk, sometimes requiring revision surgery.
Less common but more serious complications include excessive tissue removal, chronic pain, or issues affecting function.
Thorough preoperative consultation, realistic expectations, careful surgical planning, and strict adherence to post-operative instructions all play a critical role in minimizing risks and achieving a safe, satisfactory outcome.

Conclusion
In conclusion, labiaplasty is a highly individualized surgical procedure designed to address functional discomfort, aesthetic concerns, and reconstructive needs while preserving normal sensation and anatomy. When performed for appropriate reasons and by a qualified, experienced surgeon, the procedure can provide meaningful improvements in comfort, confidence, and overall quality of life. A successful outcome relies on thorough preoperative evaluation, clear communication of goals and expectations, meticulous surgical technique, and careful post-operative care.
Read More
