A cornea transplant is a surgical procedure used to restore vision by replacing a damaged or diseased cornea with healthy donor tissue.
What is a cornea transplant?
A cornea transplant is a surgical procedure in which a damaged or diseased cornea is replaced with healthy donor tissue to restore clearer vision and improve eye comfort. The cornea is the transparent, dome‑shaped surface at the front of the eye that helps focus light, and when it becomes scarred, swollen, or misshapen, vision can become blurry or distorted. Conditions such as keratoconus, infections, injuries, or inherited disorders may cause corneal damage that cannot be corrected with glasses, contact lenses, or other treatments. During a transplant, an eye surgeon removes either the full thickness of the cornea or only the affected layers, depending on the specific problem. Modern techniques allow for highly targeted approaches, which can lead to faster healing and better visual outcomes. After the donor tissue is placed, tiny stitches or specialized techniques secure it in position. Recovery involves using eye drops, protecting the eye from injury, and attending regular follow‑up visits to monitor healing. While all surgeries carry risks, cornea transplantation is one of the most successful and commonly performed transplant procedures, offering many people the chance to regain clearer vision and improve their quality of life.
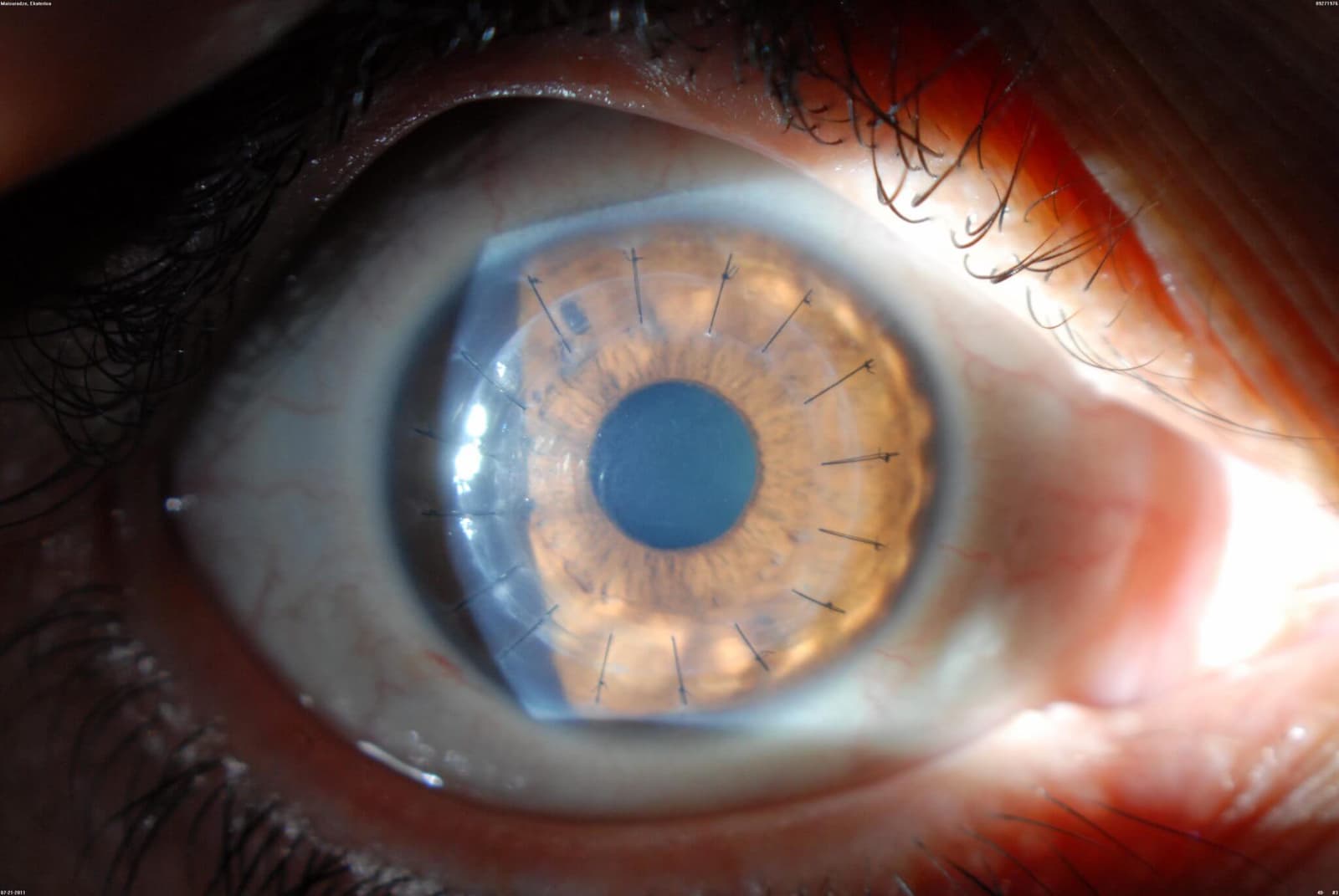
Why is cornea transplant done?
A cornea transplant is performed to restore clearer vision, reduce pain, and improve eye health when the cornea becomes too damaged to function properly. The cornea plays a crucial role in focusing light, and when it becomes cloudy, scarred, or misshapen, vision can decline to the point where glasses, contact lenses, or other treatments are no longer effective.
One of the most common reasons for a cornea transplant is keratoconus, a condition in which the cornea thins and bulges outward, causing significant distortion.
Transplants are also used to treat corneal scarring from infections, such as severe keratitis, or injuries that leave permanent marks.
Inherited disorders like Fuchs’ endothelial dystrophy can cause the inner layer of the cornea to fail, leading to swelling and blurred vision that often requires surgical replacement.
Some people need a transplant after previous eye surgeries that damaged the cornea or when long‑term swelling does not improve with medication. In these situations, replacing the affected layers—or the entire cornea—can restore clarity and comfort.
Because modern techniques allow surgeons to target only the damaged portions, many patients experience faster healing and better visual outcomes, making cornea transplantation a highly effective treatment for a wide range of corneal diseases.
What are the different types of cornea transplant surgeries?
Several types of cornea transplant surgeries exist today, each designed to target specific layers of the cornea and address different causes of vision loss.
The traditional approach is penetrating keratoplasty (PK), a full‑thickness transplant in which the entire damaged cornea is replaced with healthy donor tissue. PK is often used when scarring or disease affects all layers of the cornea. More modern techniques focus on replacing only the affected layers, which can lead to faster healing and fewer complications.
Deep anterior lamellar keratoplasty (DALK) removes the front and middle layers of the cornea while preserving the patient’s healthy inner layer, making it useful for conditions like keratoconus. For diseases affecting the innermost layer, surgeons use endothelial keratoplasty.
Two common forms are Descemet’s stripping endothelial keratoplasty (DSEK) and Descemet’s membrane endothelial keratoplasty (DMEK). DSEK replaces a thin layer of donor tissue that includes endothelium and some supporting tissue, while DMEK uses an even thinner, more precise graft consisting only of the donor’s Descemet’s membrane and endothelium.
These partial‑thickness procedures typically offer quicker visual recovery, less risk of rejection, and improved long‑term outcomes. The choice of surgery depends on which corneal layers are damaged and the patient’s overall eye health.
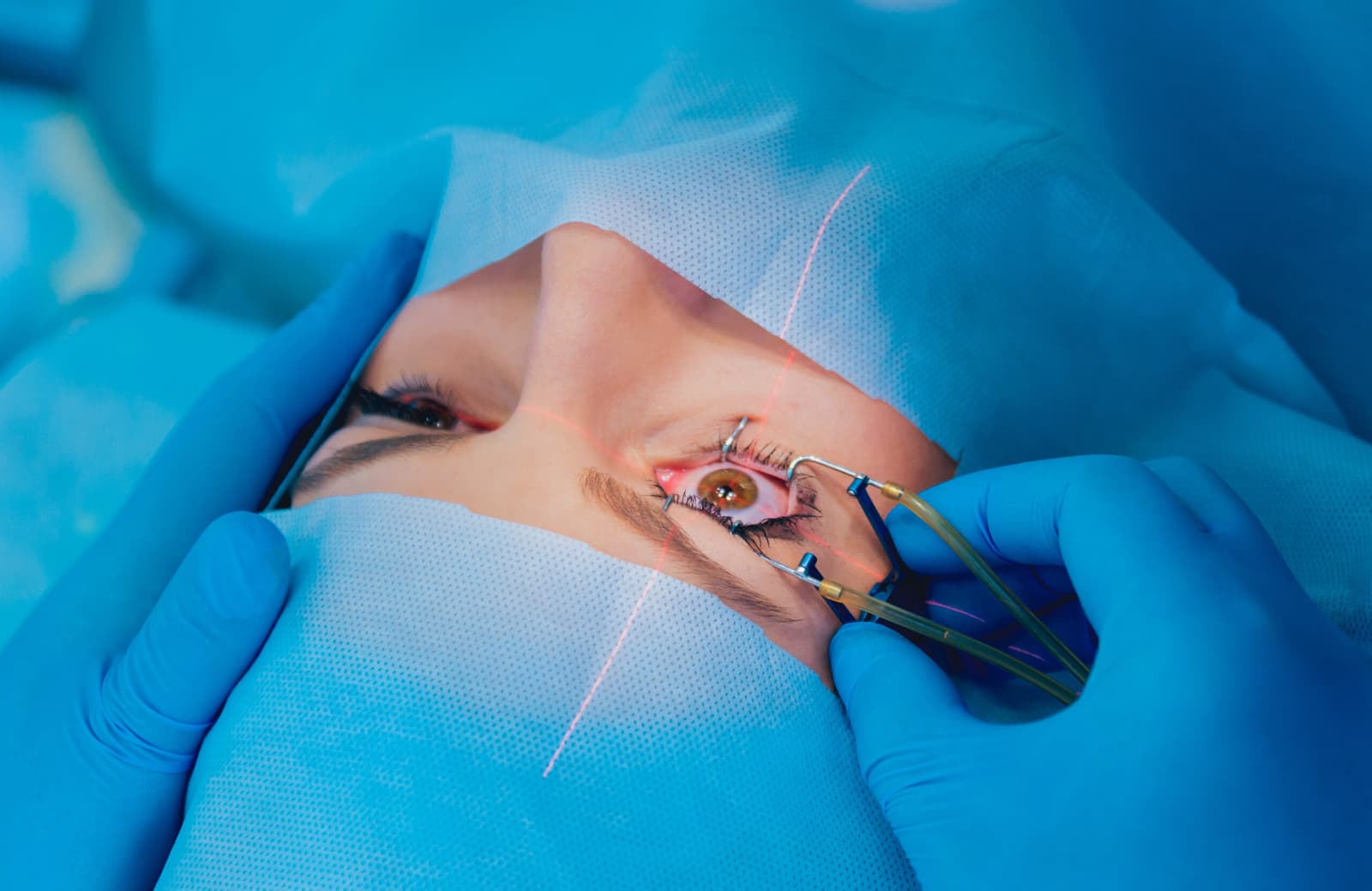
How to prepare for a cornea transplant?
Preparing for a cornea transplant involves a combination of medical evaluations, practical planning, and personal readiness to ensure the safest possible surgery and recovery. Before the procedure, patients undergo a thorough eye examination to confirm the type and extent of corneal damage and to determine which transplant technique is most appropriate. Additional tests may include measurements of eye pressure, imaging of the cornea, and assessments of overall eye health. Doctors also review medical history, current medications, and any underlying conditions that could affect healing. In some cases, patients may need to adjust or temporarily stop certain medications under medical guidance. Preparing for surgery also means arranging transportation, planning time off from work or school, and organizing help at home for the first few days after the procedure. Patients are usually advised to avoid wearing contact lenses for a period before surgery and to follow specific instructions about eating, drinking, and using eye drops on the day of the operation. Emotional preparation matters too, as understanding the procedure and recovery process can help reduce anxiety. By taking these steps and maintaining close communication with the eye care team, patients set the stage for a smoother surgery and a more successful healing experience.
What happens during a cornea transplant?
During a cornea transplant, an eye surgeon replaces the damaged or diseased portion of the cornea with healthy donor tissue to restore clearer vision and improve eye comfort. The procedure begins with numbing the eye using local anesthesia, sometimes combined with sedation to help the patient relax. Once the eye is prepared, the surgeon uses a precise instrument to remove either the full thickness of the cornea or only the affected layers, depending on the specific condition being treated. In a full‑thickness transplant, a circular section of the cornea is removed and replaced with a matching donor graft. In partial‑thickness procedures, such as DSEK, DMEK, or DALK, only selected layers are replaced, allowing the surgeon to preserve healthy tissue. The donor tissue is then carefully positioned and secured—either with tiny stitches in full‑thickness transplants or with specialized techniques, such as air or gas bubbles, in endothelial procedures. Throughout the surgery, the surgeon ensures the graft is centered, smooth, and functioning properly. The procedure typically takes one to two hours, after which the patient goes home the same day with protective shielding and detailed instructions for eye drops and care. Early healing begins immediately, though full visual recovery can take weeks to months depending on the type of transplant.
What are the risks & complications of cornea transplant?
A cornea transplant is generally considered one of the most successful transplant procedures, but like any surgery, it carries risks and potential complications that patients should understand. One of the most significant concerns is graft rejection, which occurs when the immune system recognizes the donor tissue as foreign and begins to attack it. Symptoms such as redness, sensitivity to light, decreased vision, or pain require prompt medical attention to protect the graft. Infection is another possible complication, as the eye is vulnerable during the healing period; careful use of prescribed eye drops helps reduce this risk.
Some patients may experience increased eye pressure, which can lead to glaucoma if not managed appropriately. Other complications include swelling of the cornea, delayed healing, or problems related to stitches in full‑thickness transplants. In partial‑thickness procedures, the donor tissue may shift or detach, requiring additional treatment. Vision may fluctuate for several months, and some patients still need glasses or contact lenses after healing. Although these risks exist, most complications can be managed effectively with early detection and proper follow‑up care. Regular check‑ups, consistent use of medications, and protecting the eye from injury all play important roles in ensuring a successful outcome after cornea transplantation.
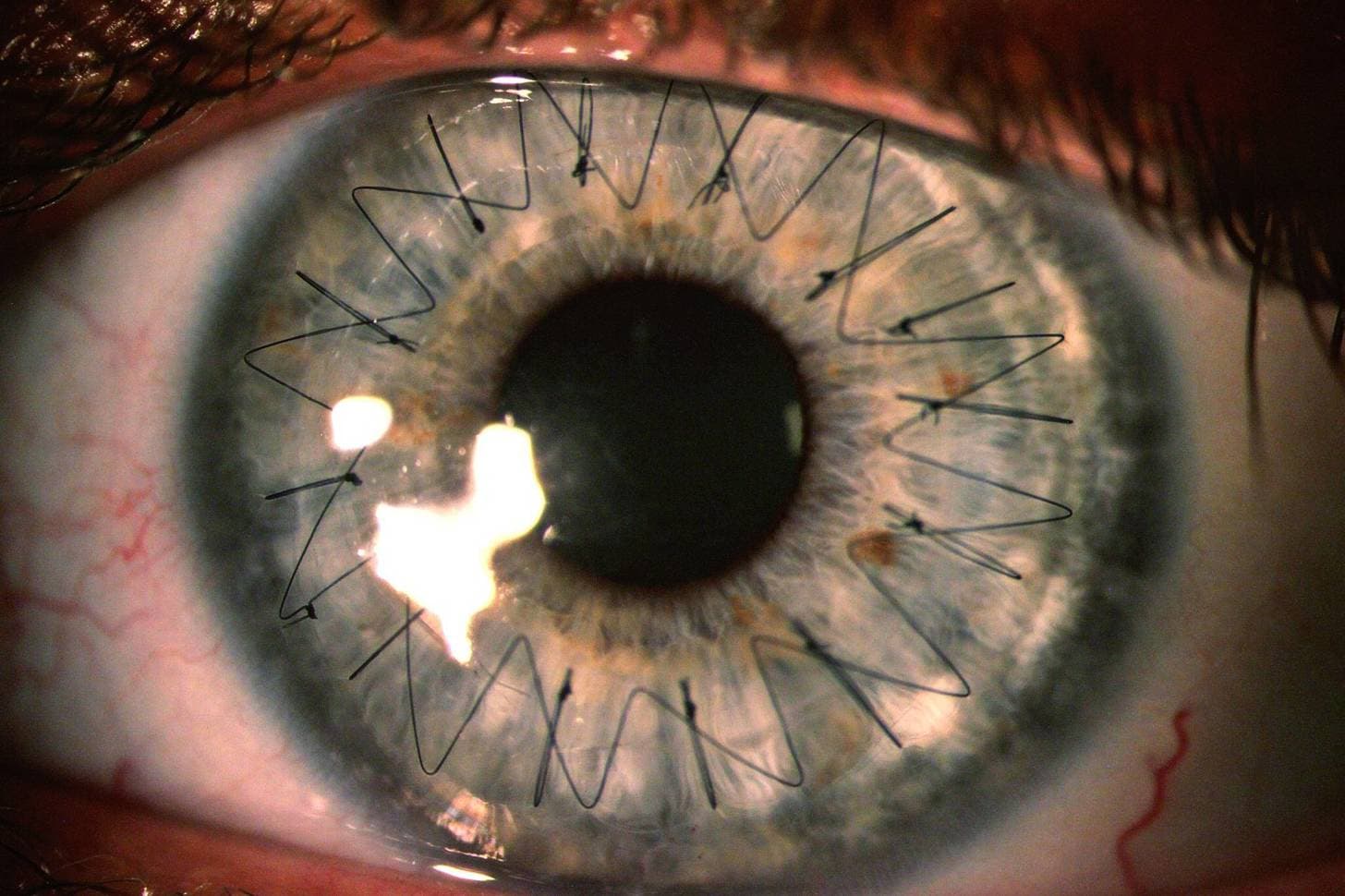
Cornea transplant recovery
Cornea transplant recovery is a gradual process that requires patience, consistent follow‑up, and careful protection of the healing eye. Immediately after surgery, patients typically go home the same day with a protective shield and detailed instructions for using prescribed eye drops, which help prevent infection and reduce inflammation. Vision is often blurry at first, and it may take weeks to months for clarity to improve, depending on the type of transplant performed. Full‑thickness procedures generally require longer healing times, while partial‑thickness techniques like DSEK, DMEK, or DALK often allow for faster visual recovery. During the early weeks, patients must avoid rubbing the eye, lifting heavy objects, or engaging in activities that could cause injury or pressure changes. Regular follow‑up visits are essential so the surgeon can monitor healing, adjust medications, and check for early signs of complications such as graft rejection or increased eye pressure. Stitches from full‑thickness transplants may remain in place for months and are removed gradually as the eye stabilizes. Most people eventually return to normal routines, though some may still need glasses or contact lenses for the best vision. With proper care and close communication with the eye care team, cornea transplant recovery can lead to significant and lasting improvements in sight.
Conclusion
A cornea transplant offers a meaningful opportunity to restore clearer vision and improve overall eye comfort when other treatments are no longer effective. Thanks to modern surgical techniques and careful postoperative care, many people experience significant and lasting improvements in their sight. While recovery takes time and requires ongoing follow‑up, the procedure has a strong track record of success and can greatly enhance daily functioning and quality of life. For individuals with advanced corneal disease, a transplant can be an important step toward regaining visual clarity and confidence in everyday activities.
Read More
