Prostate surgery encompasses a range of procedures used to treat benign prostatic hyperplasia (BPH) and prostate cancer, with choices driven by the underlying diagnosis, prostate size, symptom severity, patient health, and treatment goals.
What is The Prostate?
The prostate is a small, walnut‑sized gland in the male reproductive system located just below the bladder and surrounding the prostatic portion of the urethra; composed of glandular and muscular tissue, it contributes fluid to semen that nourishes and helps transport sperm, and its muscular contractions assist ejaculation. Structurally the prostate is organized into zones and lobes with a rich blood supply, venous plexus, and autonomic innervation that regulate secretory function and urinary control. The gland normally enlarges with age, a process that can narrow the urethral lumen and produce lower urinary tract symptoms such as weak stream, urgency, nocturia, and incomplete emptying. The prostate is also the site of common clinical conditions including benign prostatic hyperplasia, prostatitis (inflammatory or infectious), and prostate cancer, each with distinct implications for urinary function, sexual health, and systemic wellbeing. Clinical evaluation of the prostate may include digital rectal examination, prostate‑specific antigen testing, imaging, and biopsy when indicated. Because the prostate sits at the junction of urinary and reproductive tracts, disorders of the gland can affect both urinary flow and reproductive function, and management balances symptom relief, preservation of quality of life, and disease‑specific treatment goals.
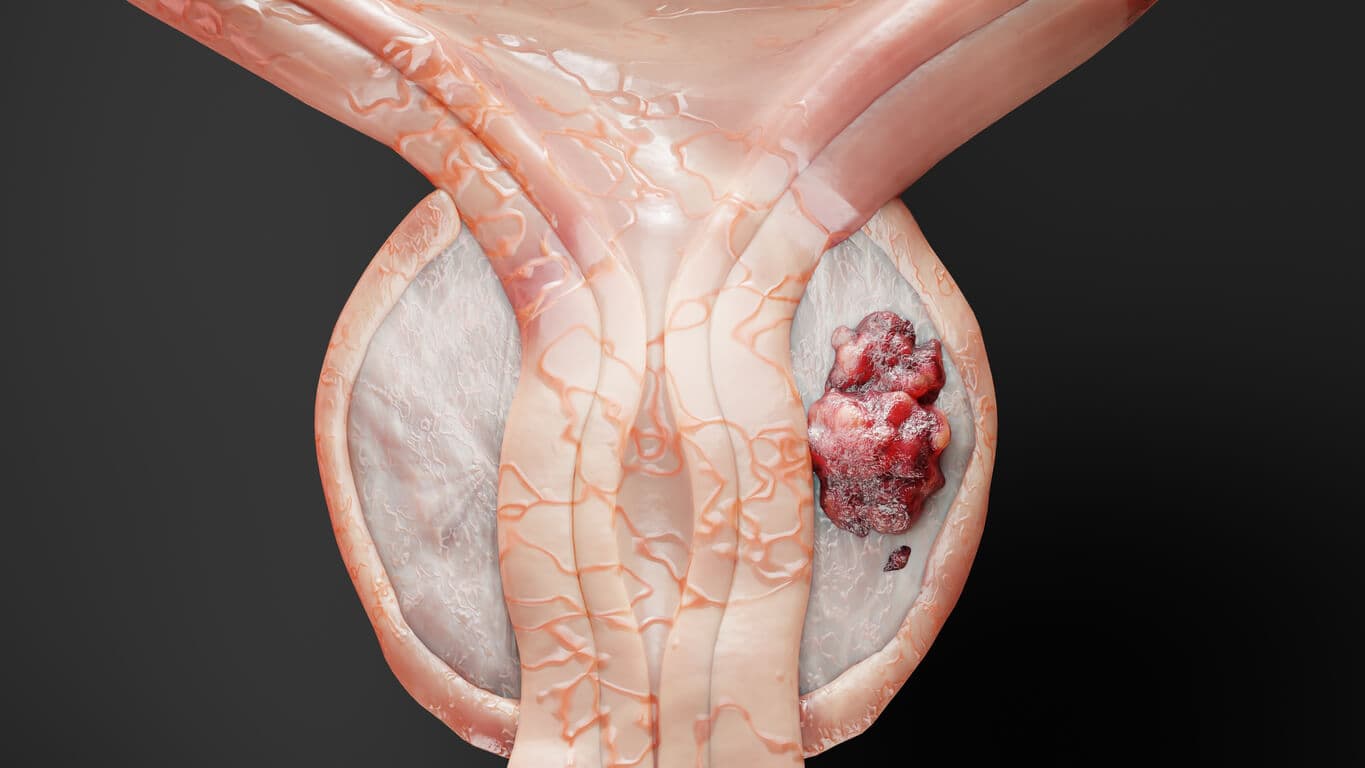
The Different Types of Prostate Surgery
Prostate surgery encompasses several distinct procedures tailored to the underlying disease—benign prostatic hyperplasia (BPH) or prostate cancer—and to gland size, symptom burden, and patient goals; three widely used approaches are radical or simple prostatectomy, holmium laser enucleation of the prostate (HoLEP), and transurethral resection of the prostate (TURP).
Prostatectomy, which may be performed as a radical prostatectomy for cancer or as a simple (open or minimally invasive) prostatectomy for very large benign glands, involves removal of prostate tissue to achieve oncologic control or relieve obstruction; radical prostatectomy removes the entire gland and seminal vesicles and can be done via open, laparoscopic, or robot‑assisted approaches with the aims of cancer eradication and preservation of urinary continence and sexual function when feasible, while simple prostatectomy removes only obstructing adenomatous tissue and is reserved for glands too large for endoscopic techniques.
HoLEP is a minimally invasive, endoscopic laser enucleation technique that uses a holmium laser to dissect and remove the obstructing adenoma from the surgical capsule, offering durable relief of obstruction across a wide range of prostate sizes with low retreatment rates and the advantage of reduced bleeding compared with traditional resection; tissue is morcellated and removed, allowing histologic examination and making HoLEP particularly useful for large glands where TURP would be impractical.
TURP, long considered the gold standard for moderate‑sized prostates, is an endoscopic procedure in which a resectoscope is passed through the urethra and electrocautery is used to shave away obstructing tissue, producing rapid symptomatic improvement and urinary flow restoration but carrying risks such as bleeding, TUR syndrome in older irrigation systems, and a high likelihood of retrograde ejaculation.
Choice among these procedures depends on prostate size, anticoagulation status, patient comorbidities, and priorities such as preservation of ejaculation or minimizing hospital stay.
What are the common Side Effects of Prostate Surgery?
Prostate surgery commonly produces a predictable set of side effects that vary with the procedure and individual factors but often include urinary incontinence, erectile dysfunction, and changes in ejaculation such as retrograde ejaculation; these functional consequences may be temporary for some patients but can be persistent and require rehabilitation or medical management.Patients also face general surgical risks—bleeding, wound or urinary tract infection, and thromboembolic events—which are managed with perioperative precautions and prompt treatment when they occur.Endoscopic procedures such as TURP carry procedure‑specific complications including significant bleeding and, rarely with older irrigation techniques, dilutional “TUR syndrome,” while laser enucleation and newer minimally invasive approaches tend to reduce blood loss but still risk urinary irritation and catheter dependence in the short term.Beyond immediate physical effects, men may experience emotional distress, changes in body image, and fertility loss after prostate removal, so counseling and access to sexual‑health and psychosocial support are important parts of recovery.With careful preoperative counseling, pelvic‑floor rehabilitation, pharmacologic therapies, and, when needed, surgical revisions or devices, many side effects can be mitigated and quality of life improved.

Conclusion
Prostate surgery includes a spectrum of procedures—radical or simple prostatectomy, TURP, and HoLEP—each designed to address distinct goals such as cancer control, durable relief of bladder outlet obstruction, or symptom improvement with minimal invasiveness. Selecting the right approach depends on the underlying diagnosis, prostate size, patient comorbidities, and priorities around recovery, continence, and sexual function. Modern techniques offer effective outcomes with evolving tradeoffs in bleeding risk, retreatment rates, and functional side effects, so careful preoperative counseling, individualized planning, and experienced surgical teams are essential to optimize both disease control and quality of life.
Read More