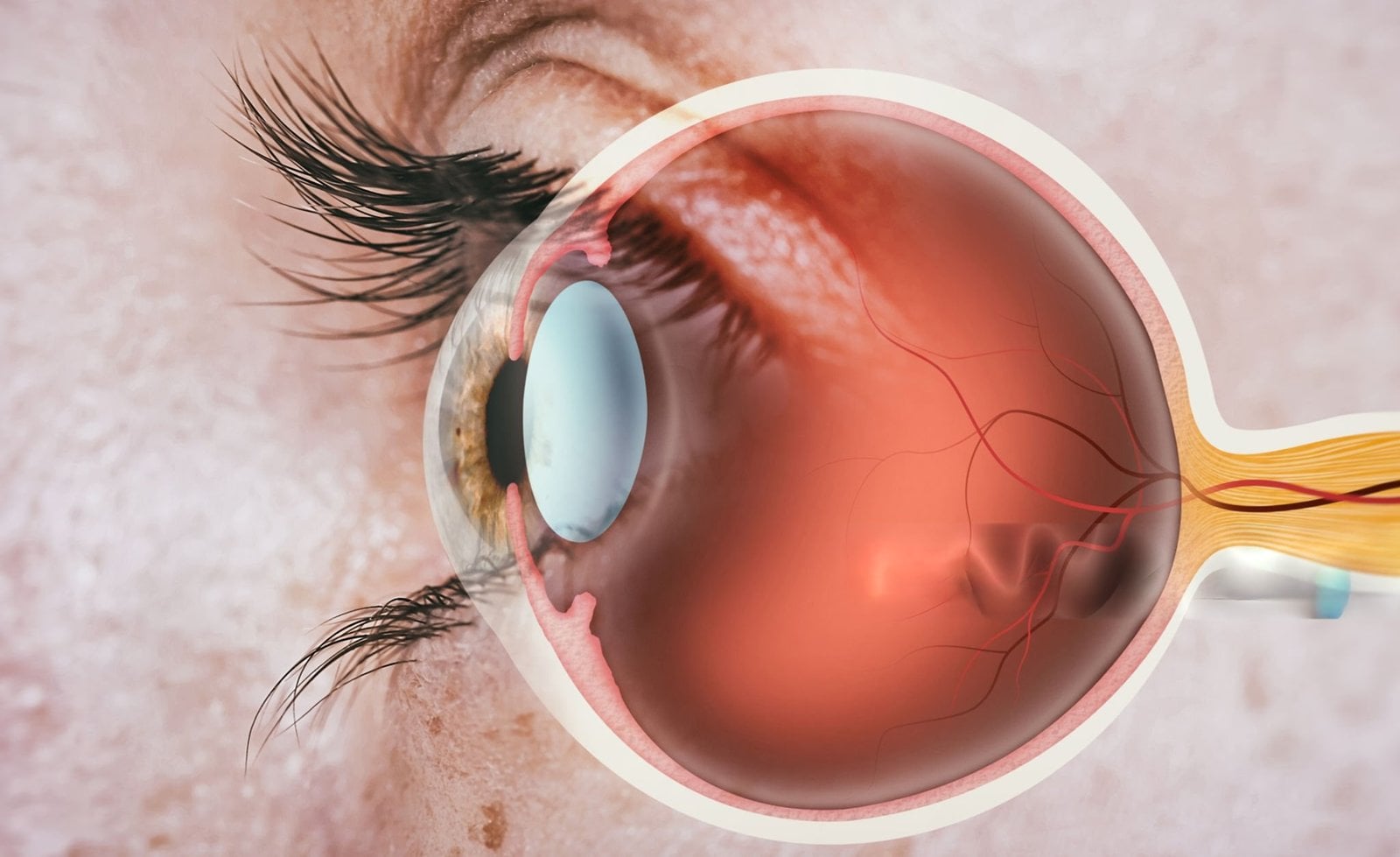
Retina surgery addresses disorders of the retina and vitreous that threaten vision, using a range of targeted techniques chosen by diagnosis, severity, and patient factors.
What is a retina surgery?
Retina surgery is a group of specialized ophthalmic procedures aimed at treating disorders of the retina and vitreous that threaten vision, such as retinal detachment, macular holes, epiretinal membranes, and complications of diabetic retinopathy.Common techniques include vitrectomy, in which the vitreous gel is removed to allow direct repair of the retina and to clear hemorrhage or traction; scleral buckle, an external support placed around the eye to close retinal breaks; and pneumatic retinopexy, where a gas bubble is injected into the eye to tamponade a retinal tear while the retina reattaches.Laser photocoagulation and cryotherapy are frequently used adjuncts to seal tears, treat proliferative disease, and reduce edema.Many retinal surgeries are urgent—particularly retinal detachment repairs—to maximize the chance of visual recovery, and the choice of procedure depends on detachment configuration, extent of disease, and patient factors.Recovery varies by operation and patient health: vision may improve gradually over weeks to months, and postoperative positioning, activity restrictions, and close follow‑up are often required to ensure anatomical success and monitor for complications.
Types of retina surgery
Retina surgery comprises a set of targeted procedures designed to treat sight‑threatening disorders of the retina and vitreous, and four commonly used approaches—pars plana vitrectomy, laser photocoagulation for retinal tears or diabetic retinopathy, scleral buckling, and pneumatic retinopexy—are selected based on the underlying pathology, detachment configuration, and patient factors;
Vitrectomy is the most versatile microsurgical technique in which the vitreous gel is removed via small trans‑scleral ports to relieve traction, clear vitreous hemorrhage, allow membrane peeling (for epiretinal membranes or macular holes), perform internal tamponade with gas or silicone oil, and directly repair complex retinal detachments or proliferative diabetic disease, offering high anatomic success especially for posterior or complex detachments but requiring intraocular tamponade and often postoperative positioning;
Laser photocoagulation uses focused thermal burns delivered through the pupil to seal retinal tears, create chorioretinal adhesions around breaks, and treat ischemic retinal areas in proliferative diabetic retinopathy or focal macular edema—laser is minimally invasive, can be performed in clinic or the operating room, and is frequently combined with other surgeries to reduce re‑detachment risk or to regress neovascularization, though it can cause peripheral visual field loss and scotomas if extensive;
Scleral buckling is an external procedure that places an encircling or segmental silicone element against the sclera to indent the eye wall, close retinal breaks, and relieve vitreoretinal traction without entering the globe, and it remains particularly useful for young phakic patients with peripheral retinal breaks and uncomplicated rhegmatogenous detachments, offering durable reattachment while avoiding intraocular tamponade but carrying risks such as induced refractive change, extraocular muscle disturbance, and longer recovery;
Pneumatic retinopexy is a minimally invasive office‑based or operating‑room technique in which a gas bubble is injected into the vitreous cavity to tamponade a superior retinal break while adjunctive laser or cryotherapy seals the tear—its advantages include rapid recovery, avoidance of scleral surgery, and suitability for selected detachments with single or few superior breaks, but it is limited by lower success rates for complex or inferior detachments and requires strict postoperative head positioning and patient cooperation.
In practice, retinal surgeons often combine modalities—performing vitrectomy with endolaser, using scleral buckle plus vitrectomy for inferior breaks, or following pneumatic retinopexy with laser—to tailor treatment to detachment extent, presence of proliferative vitreoretinopathy, lens status, and systemic considerations; perioperative planning addresses anesthesia, anticoagulation, choice of tamponade (air, long‑acting gas, or silicone oil), and patient counseling about positioning, activity restrictions, and the expected timeline for visual recovery, which can continue to improve for months.
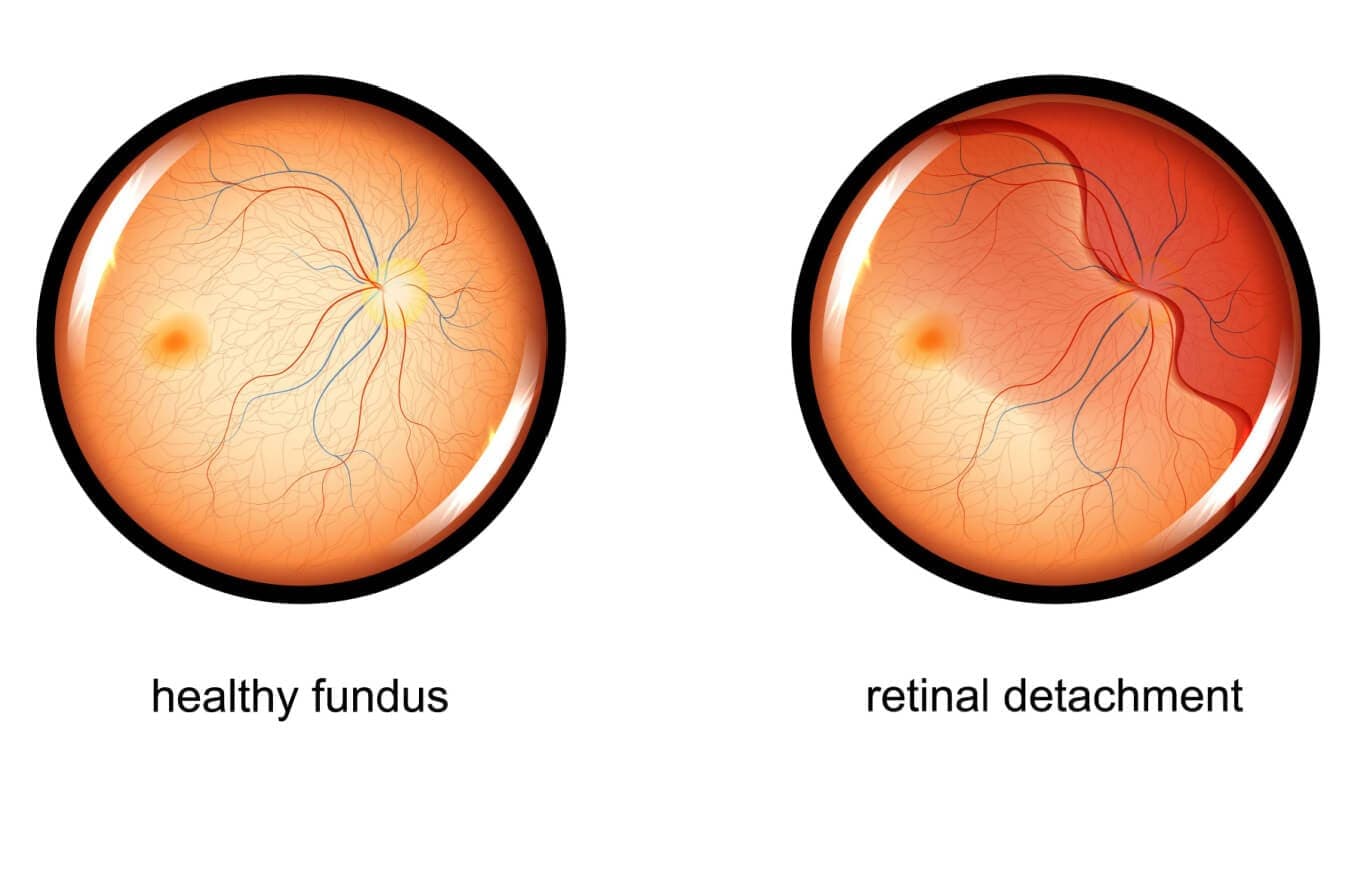
What happens during Retinal surgery?
Retinal surgery involves a sequence of precise, microsurgical steps tailored to the underlying problem—most commonly retinal detachment, vitreous hemorrhage, macular hole, or proliferative diabetic disease—and begins with anesthesia (local with sedation or general) and sterile preparation of the eye.Surgeons commonly perform a pars plana vitrectomy, creating small trans‑scleral ports to remove the vitreous gel, relieve traction, clear blood, and permit direct manipulation of the retina such as membrane peeling or laser application; intraocular instruments allow fluid–air exchange and placement of a tamponade agent (gas or silicone oil) to support reattachment.For peripheral retinal tears the surgeon may apply laser photocoagulation or cryotherapy to create chorioretinal adhesions that seal breaks and reduce the risk of recurrent detachment.In selected cases an external scleral buckle is placed to indent the globe and close retinal breaks without entering the eye, a technique still favored for certain rhegmatogenous detachments.Pneumatic retinopexy—injecting an intraocular gas bubble and then using laser or cryo to seal the tear—is an office‑based option for simple superior breaks but requires strict postoperative head positioning and patient cooperation.Throughout the procedure surgeons monitor intraocular pressure, manage bleeding, and plan postoperative care including positioning, medications, and follow‑up to detect complications and optimize visual recovery.
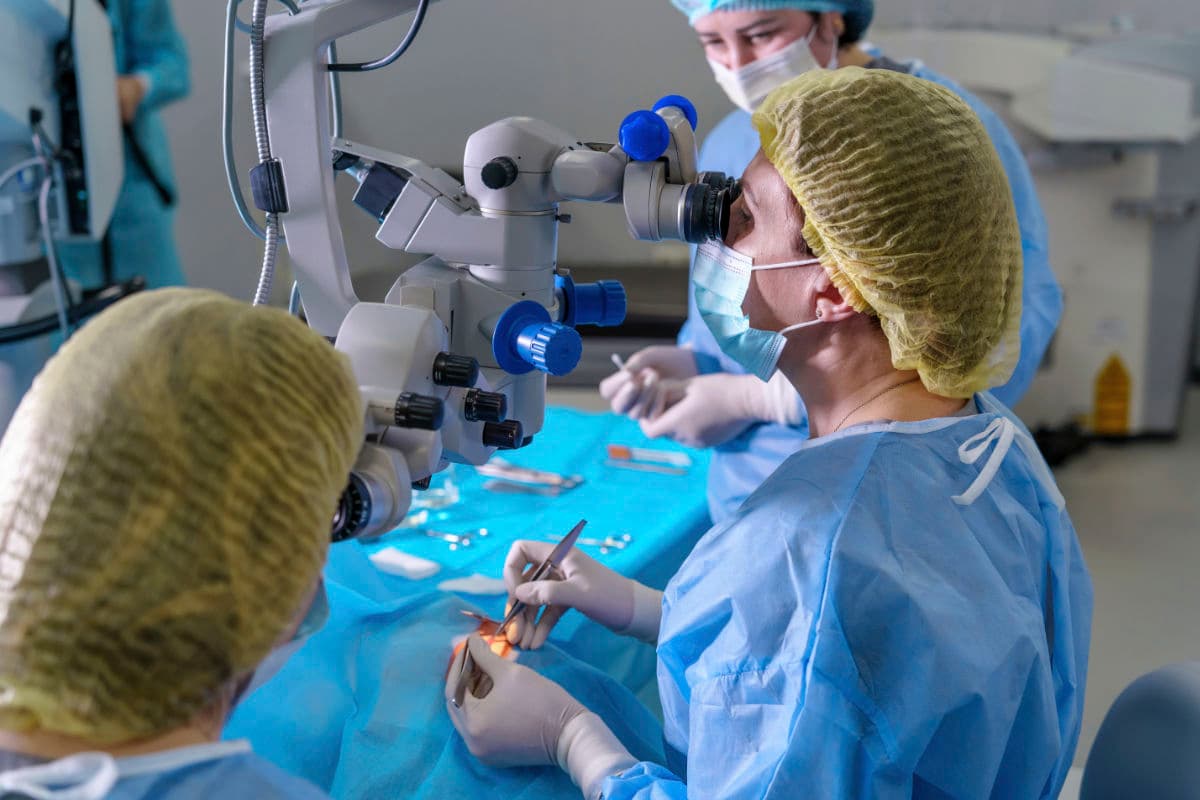
Conclusion
Retina surgery offers a range of targeted techniques—vitrectomy, laser photocoagulation, scleral buckling, and pneumatic retinopexy—each chosen to address specific retinal and vitreous problems based on anatomy, severity, and patient factors. Timely intervention by an experienced retinal specialist maximizes the chance of anatomical reattachment and visual recovery, while perioperative planning (choice of tamponade, positioning, and follow‑up) and patient cooperation are critical to success. Because procedures can be combined or sequenced to match complex presentations, individualized treatment planning and clear postoperative guidance help balance risks and benefits and optimize long‑term visual outcomes.
Read More